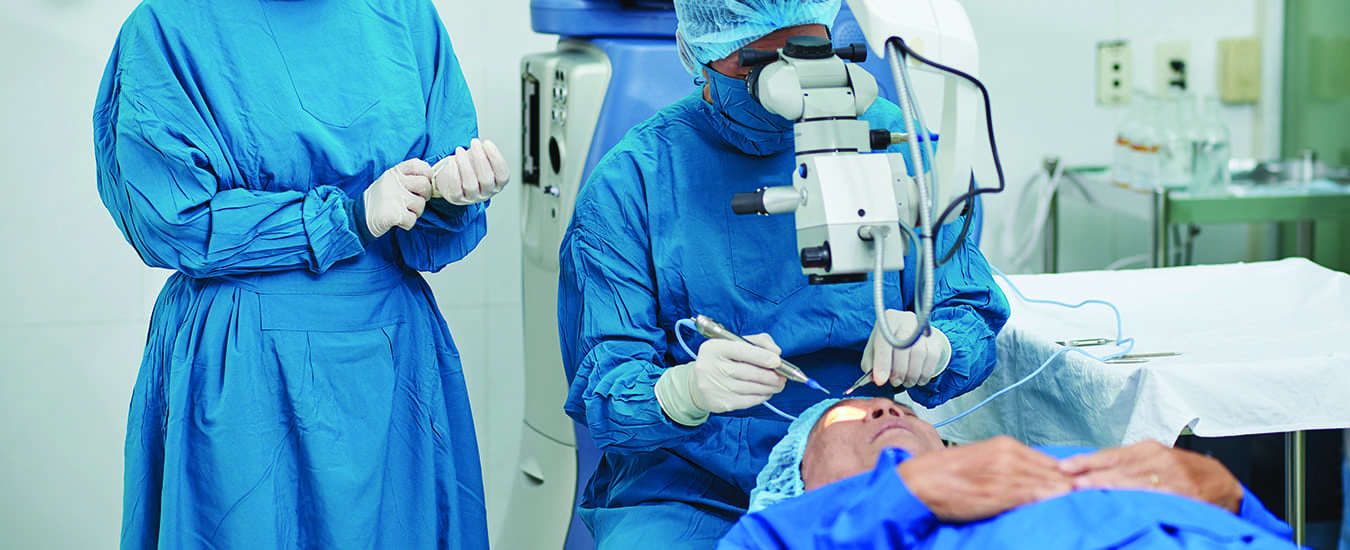
Cataract surgery is one of the most common, and effective, surgeries
The first thing Nita Whitehead noticed was that it was getting harder and harder to drive at night. Then the sun started hurting her eyes. Nita knew her vision wasn’t as clear as it had been and the situation seemed to be getting worse, so she booked an eye exam.
“The best way to describe it is that things were hazy. It was like I was always looking through a fog and everything was getting harder and harder to see, especially when I was driving, so I didn’t drive much anymore,” says Nita, 67, from Falmouth, NS. “During the daytime the sun was so hard on my eyes, even wearing sunglasses didn’t help. I had no idea what was going on but when I mentioned it to my optometrist, she said it looked like cataracts and referred me to see an ophthalmologist.”
In November 2014, Nita had cataract surgery on her right eye. One month later she had surgery on her left eye. Both surgeries were done at the Eye Care Centre in the Centennial Building of the Queen Elizabeth II Health Sciences Centre in Halifax.
“I was a bit nervous going in, but it was fast. And the difference in my eyesight was amazing. I could see better right away,” she says.
Now, more than three years later, Nita still marvels at how much better her vision is, allowing her to drive her teenage grandson, who lives with Nita and her husband Arnold, to his hockey games and to go play music. “I can drive anywhere now. It’s no problem,” she says. “It’s made such a difference, definitely for the better.”

What are cataracts?
A cataract is a clouding of the lens of the eye, causing blurred vision. In its early stages, a cataract does not cause a problem and usually is not even noticed by the person affected. Over time, however, the cataract becomes denser, causing less light to reach the retina and making it increasingly harder to see. Night vision is reduced and colours lose their brightness and contrast. And, as Nita Whitehead found out, cataracts also cause the eye to become more sensitive to glare from the sun.
For most people the development of a cataract is a normal part of aging, but cataracts can occur in a younger person as well, usually as a result of a disease, such as diabetes, or due to prolonged use of corticosteroids, or following some sort of trauma or injury to the eye.
“In almost everyone between age 50 and 60, the lens undergoes some changes,” says Dr. Dan O’Brien, an associate professor with Dalhousie University’s department of ophthalmology and visual sciences and one of the surgeons doing cataract surgery at the Eye Care Centre at the QEII. “The changes happen at such a slow rate you don’t even notice it until eventually you have some difficulty seeing. That’s really when we start talking about the development of the cataract, but the actual changes occur much earlier than that.”
Usually, unless the cataract has been caused by trauma to an eye, both eyes develop cataracts at about the same rate. Once cataracts have been diagnosed, for many patients the next step is surgery, but not for all, explains Dr. O’Brien.
“With an early cataract, sometimes a small change in the person’s glasses can make a difference, but once the cataract advances the glasses won’t make much of a difference,” he says. “A cataract doesn’t harm or injure the eye in any way so really there is no urgency to remove it. It depends on how a person is functioning, it’s all about quality of life issues so what we look at is a person’s ability to read, to drive, to do their job and to do their hobbies.”
Screening for cataracts is part of a regular eye exam done by an optometrist. If a problem is detected, the patient is referred to an ophthalmologist for further investigation and to discuss whether surgery is needed.
Altered circumstances
Driving is one of the biggest issues for many who have cataracts, and not just increased difficulty when driving at night. To maintain your driver’s licence, Dr. O’Brien explains, there’s a legal requirement, to be able to see a certain line on the eye chart. “If the person can’t see that line there’s a choice to make and that choice is either to stop driving or to have the cataract removed. Most people don’t want to lose their licence, as it’s their independence, and will opt for surgery.”
Being told you can no longer drive can be an unpleasant shock, as Tania Basic found out earlier this year. The 56-year-old had made an appointment with her optometrist because she’d been having some trouble with her vision. Her main symptom was decreased night vision. “Tail lights and headlights just looked like a starburst,” she says.
Tania was shocked when she was found out how poor her vision had become; she failed the eye exam and was told she could no longer legally drive. Tania was referred to an ophthalmologist and waited anxiously for that appointment. With two sons still living at home (only one of whom has his driver’s licence) and a husband who works away a lot, Tania was concerned how she would manage to maintain the lifestyle she and her family loved in their Hammonds Plains home.
“I was worried that it could be something really serious, even blindness. I couldn’t imagine losing my vision and living where I do now. It’s a half hour walk to the nearest bus stop and there’s no sidewalks,” she says. “When the ophthalmologist told me was cataracts and could be fixed by surgery, it was a complete relief.”
Cataract surgery
According to Dr. O’Brien, most people over the age of 60 have cataracts. Not all of those people go on to have surgery, but once the condition gets to the point that it’s interfering with their quality of life, surgery is the only available option. Cataract surgery is one of the most common surgical procedures, with about 98 per cent getting at least 20/40 vision back in their eye—legal driving vision—and some getting much better than that.
In Nova Scotia, about 10,000 cataract surgeries are performed each year, about half of them done in Halifax. Dr. O’Brien handles more complex cases and does about 600 a year, with about half his patients coming from NB and PEI.
During cataract surgery, the cloudy lens in the eye is replaced with a clear artificial lens—an intraocular lens—in a procedure called phacoemulsification. Usually, each eye is done separately, although the second procedure is generally done within weeks of the first.
Before surgery, eye drops are administered to dilate the pupil. More eye drops anaesthetize the patient’s eye before the surgeon makes tiny incision on the side of the cornea to remove the cataract and insert the new lens; there are no sutures needed. In the past, surgeons simply swapped out the cloudy lens for an artificial one, but now they also change the refractive error of the eye to just slightly near sighted—meaning many people who wear glasses won’t need them anymore, except perhaps for reading glasses. For a routine cataract surgery, the entire procedure takes between 15 minutes to half an hour.
At the Eye Care Centre at the QEII, cataract surgeons do between 12 to 16 surgeries per day in two separate “cataract rooms,” Dr. O’Brien says, with two other rooms for more complex eye issues. “The staff at the Eye Care Centre run a very efficient system.”
As was the case with both Nita and Tania, most people who get the surgery notice a marked improvement in their vision right away.
“It’s something we call the ‘wow factor’,” says Dr. O’Brien. “When you develop cataracts, it usually comes on so slowly and so gradually, you just adapt to the situation until you get to the point where you’re having difficulty reading or driving. When the surgery is done there’s an almost instantaneous recovery of vision. Right away, people go “wow,” and say that they had no idea how bad their vision was.”
During recovery after surgery, patients are given an eye shield to wear home to protect their eye as most experience itchiness in their eye for a short while following the procedure. Patients continue to wear the shield at night for a couple of weeks, or until the eye is no longer itchy.
Tania had minimal discomfort following her surgery and says she is amazed at the difference in her vision. “The clarity was unbelievable. Now, when I look through my eye that hasn’t been done yet, it’s like looking through a dirty window. I had no idea how bad my eyes were. Everything is so sharp and vivid. The colours are brighter and everything is clearer. It’s a huge gift.”
Following her surgery, Tania was relieved when she got the news she would be allowed to drive again. “My licence has been re-instated. I am completely elated.”
What causes cataracts?
- Age: Age is the most common cause of cataracts.
- Trauma: Injury or damage to the eye can cause a cataract to develop.
- Medications: prolonged corticosteroid use is linked to cataracts.
- Disease: Systemic diseases, such as diabetes, increases the risk that a cataract will develop.
- Too much sun exposure: Prolonged exposure to ultraviolet light may put you at a higher risk.
- Smoking: People who smoke seem to get cataracts earlier than non-smokers.
Source: Canadian Ophthalmological Society
What are the symptoms of cataracts?
Each person may experience symptoms differently; early symptoms may include:
- Blurry vision
- Glare, particularly at night
- Change in your eyeglass prescription, such as a change from being farsighted to nearsighted
- Decrease in colour intensity; colours seem faded
- A yellowing of images
- Double vision (rare)
Source: Canadian Ophthalmological Society